Unsanitary conditions put nursing home residents at risk of serious infections, which can lead to lengthy hospital stays, disability, and increased medical expenses. But federal law requires that nursing homes and assisted living facilities that accept Medicare maintain adequately clean and sanitary conditions.
When long-term care facilities violate these standards, and residents are injured, family members and loved ones have every right to contact a nursing home sexual abuse lawyer.
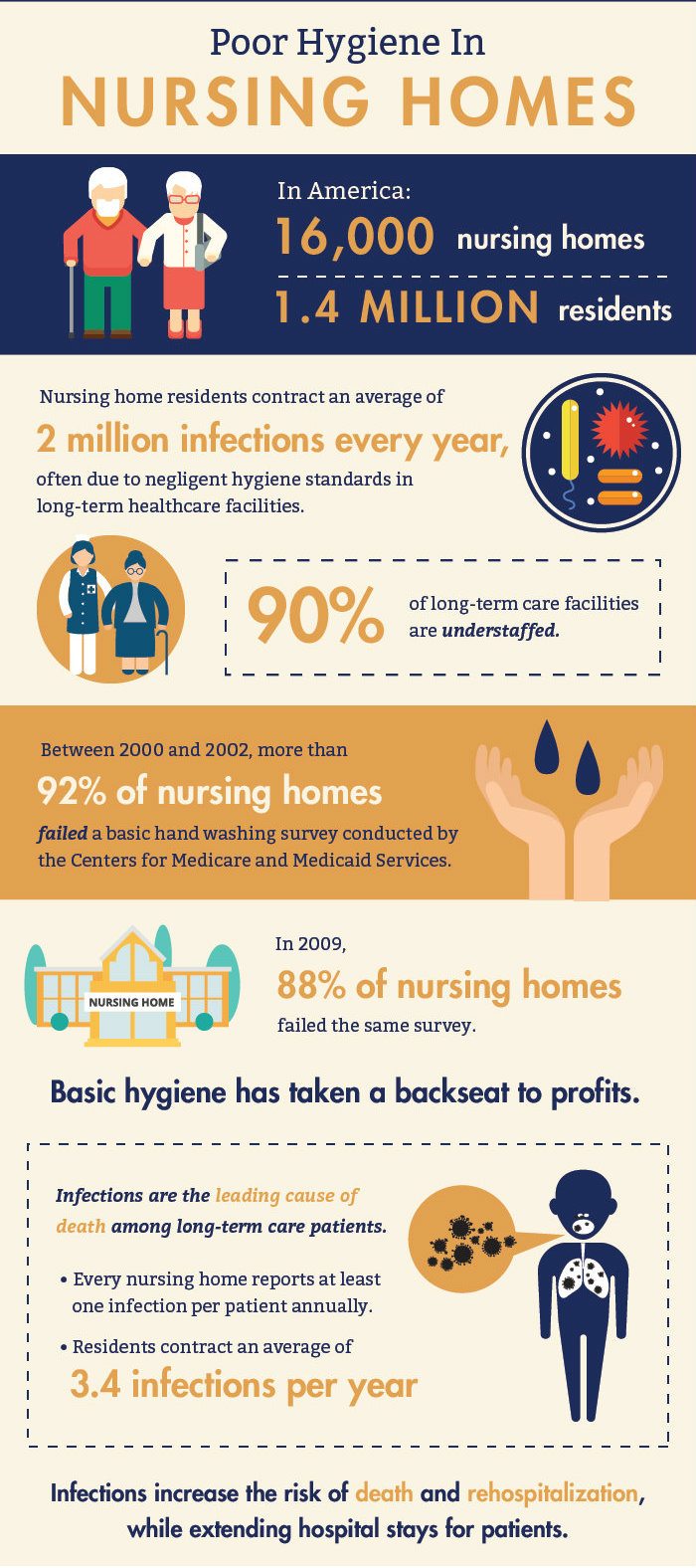
In nursing homes across the country, poor hygiene is a leading indicator of resident neglect. Long-term care facilities are chronically understaffed, and overworked nursing assistants are liable to leave elderly residents living in unclean – and unsafe – environments for months at a time. In many cases, their immoral lack of attention and care rises to the level of negligence – making a viable nursing home lawsuit possible.
Nursing homes have an incredibly high employee turn-over rate. A single nursing home may have an entirely new staff every year, according to researchers at the University of California, Irvine. With few employees staying longer than a year, nursing homes often have trouble training new staff members properly, which can have a major impact on resident health. Improper hygiene often rises to the level of a facility-wide problem, rather than remaining an issue with one or two isolated employees.
Nursing home residents contract an average of 2 million infections every year, according to researchers at the University of Michigan.
In fact, studies show that each nursing home resident can expect to develop more than one infection every year – as a matter of course. With vulnerable immune systems, many nursing home residents are unable to keep up with their own personal hygiene. That means nurses, doctors, and other facility workers need to play close attention to the hygiene of the elderly patients in their charge and assist patients in keeping clean. But in too many long-term care facilities, our elders are being neglected.
Resident cleanliness is only one part of the struggle against deadly infectious diseases in nursing homes. Nurses, nursing assistants, and other staff members have a legal responsibility to keep themselves clean as well. Tragically, this responsibility is not being honored.
Even the simplest, and most obvious, hygiene practices can be neglected in a long-term care facility. Shockingly, many nurses and employees just aren’t washing their hands before tending to residents, increasing the risk of spreading deadly infections.
Between 2000 and 2002, over 92% of nursing homes failed a basic hand washing survey conducted by the Centers for Medicare and Medicaid Services. That result was unacceptable, but change has been slow. In 2009, the survey was repeated. Only 12% of nursing homes passed the test. In 88% of the long-term care facilities studied, nurses were observed touching and treating vulnerable residents – without having followed the proper hygiene protocols beforehand.
The need for strong hygiene programs is obvious, but few long-term care facilities have been willing to take the initiative.
The vast majority of nursing homes and assisted living facilities are simply unclean. With poor hygiene a growing problem in America’s long-term care facilities, residents are being left at an increased risk of suffering devastating – but entirely preventable – infections, like:
As you may have noticed, nursing home residents aren’t just at risk of contracting minor infections. Patients in long-term care facilities are threatened by the most dangerous infectious agents in the world, including bacteria that have become resistant to antibiotics.
In fact, many elders living in nursing homes already have these devastating infections, according to a recent paper published in the journal Clinics in Geriatric Medicine. More than 1 out of 3 elderly nursing home residents are currently harboring bacteria that have become resistant to multiple antibiotics. In short, nursing homes are breeding grounds for potentially-deadly “super bugs,” like MRSA, which are extremely difficult to treat.
To compound the problem, infections are often harder to diagnose in elderly patients. The most common symptoms of an infection, like fever and white blood cell increases, are often absent in older people. This means even treatable infections can be left without proper medical attention, increasing patient discomfort and leading to chronic ill-health and higher rates of hospitalization. Death is the tragic consequence for some elders. In fact, the American Academy of Family Physicians says that one-third of all deaths among people 65 or older are attributed to infections.
Most of the common signs and symptoms of an infection are actually caused by the immune system as it struggles to fight off a foreign bacteria or virus. In young patients, fever, headaches, and pain are quite common. But many elderly patients have weakened immune systems, and won’t exhibit the same signs and symptoms that a younger patient would.
Instead, loved ones should be on the lookout for “non-specific” signs, including:
Often, physicians are given no more of a warning than an overall functional decline, a sudden or gradual impairment in an elderly patient’s ability to perform normal tasks. Dressing, use the bathroom, and bathing may appear unusually difficult.
Be particularly vigilant when your loved one has to use a catheter and after surgical operations. Elderly patients are at an increased risk of developing an infection after suffering wounds or having their internal organs exposed to the outside world.
We expect long-term health facilities to be clean. It’s natural to expect that normal hygiene practices will be followed. After all, the connection between poor hygiene and multiple life-threatening diseases has a long, deadly history. People who already have weakened immune systems may be at a severe risk, and the elderly are especially vulnerable.
When an elderly loved one is turned over to the care of others in a nursing home, there is a duty to treat that person well. Sadly, this duty is not always respected. It’s urgently important for family and loved ones to address poor hygiene conditions immediately. Patients themselves are often completely powerless in the nursing home environment, which makes the situation even more disgraceful.
Beyond infections, elderly nursing home residents are particularly susceptible to suffering from:
These health conditions put both patients and visitors at an increased risk for more serious complications. In some cases, the conditions can be brought back to the family home and the surrounding neighborhood.
Living in chronically unclean conditions can also inflict psychological trauma on nursing home residents, many of whom already live with dementia. An unsanitary environment is demeaning, an affront to the principle that every elder in our society should be able to live out their years in dignity. When elderly residents feel neglected, they may suffer from psychological effects such as increased depression and reduced enjoyment of life.
There are numerous reasons for poor hygiene to develop in a nursing home facility. Some reasons from past history include:
Nursing homes didn’t start out understaffed, and they weren’t forced to hire unqualified staff members. In most cases, these were very intentional choices made by long-term care facilities in an attempt to lower costs. But you’re paying for a standard of care that is normal and necessary for a healthy living environment during your loved one’s final years. Poor hygiene is more than economically unfair; it’s morally outrageous.
There is no time to waste when it comes to poor hygiene at a nursing home. Long-term care facilities that fail to uphold basic hygiene standards can be held responsible for neglecting residents in a court of law. But your family will need professional nursing home neglect lawyers with experience in these situations to find the truth.
Protect your loved one’s rights and dignity. Our experienced attorneys know what to look for and how to preserve evidence of poor hygiene in nursing homes. We have to stop the abuse of the elderly now. We owe it to ourselves and future generations.
Learn more about: Unexplained Cuts & Bruises A Sign Of Abuse In Nursing Homes